Ulcers after bariatric surgery are most common after the gastric bypass, although they may also occur after a gastric sleeve, a duodenal switch, or a gastric band. An ulcer is a sore in the stomach lining that, if left untreated, can cause pain, bleeding, or even result in perforation (a hole).
The incidence of ulcers after a gastric bypass is relatively low, occurring in 1 to 16% of patients, and is one of the late complications a patient may experience after gastric bypass surgery. Typically, an ulcer will occur three months from surgery in 30% of patients, four to 12 months from surgery in 23% of patients, and 12 months from surgery in 47% of patients.
Most ulcers occur at the incision site and around the staple lines and are a common reason for nausea and vomiting after gastric bypass surgery. The factors contributing to ulcerative formation after gastric bypass are not entirely clear; however, they are believed to be multifactorial.
Causes of Ulcers after Bariatric Surgery
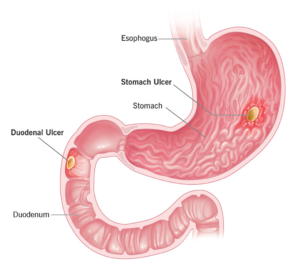 Although the factors that cause ulcers after bariatric surgery are inconclusive, some surgeons believe they may be caused by increased acid production in the new pouch, particularly the new gastric bypass pouch. There is also speculation that ulcers are caused by other gastric irritations, such as smoking or NSAIDs (non-steroidal anti-inflammatory) like aspirin and ibuprofen.
Although the factors that cause ulcers after bariatric surgery are inconclusive, some surgeons believe they may be caused by increased acid production in the new pouch, particularly the new gastric bypass pouch. There is also speculation that ulcers are caused by other gastric irritations, such as smoking or NSAIDs (non-steroidal anti-inflammatory) like aspirin and ibuprofen.
Smoking increases the risk of developing an ulcer by limiting oxygen flow to the stomach tissue. In a healthy adult, ulcers heal naturally by pumping blood to the stomach. After gastric bypass surgery, though, the smaller stomach limits blood flow. And coupled with the oxygen limitation, ulcerative healing is significantly impacted.
Researchers have recently found that the prevalence of helicobacter pylori (H. pylori) bacteria may also increase the risk of developing an ulcer after gastric bypass surgery. Nearly 25% of pre-op bariatric patients have H-Pylori in the gut; therefore, when we perform your pre-operative EGD, we will be looking for any signs of this bacteria.
Although the prevalence of H-Pylori bacteria in the stomach is not deadly, it can lead to uncomfortable symptoms such as aches or burning sensations in the abdomen, nausea, vomiting, loss of appetite, reflux, and bloating.
Symptoms of Ulcers
The typical signs and symptoms of ulcers after bariatric surgery are abdominal pain, commonly located in the epigastric region (which is the region situated right below the breast bone). Often there is also an association with food intolerances such as the inability to eat or foods you previously tolerated now causing pain.
Most commonly, when a patient complains of these types of symptoms will do an upper endoscopy scope down the mouth into the gastric bypass pouch to make the diagnosis.
Treatment for Ulcers
The treatment for ulcers is typically anti-acid medications, sometimes referred to as proton-pump inhibitors. Your physician may also prescribe Carafate to help treat your ulcer.
Most of the time, ulcers after gastric bypass surgery will heal on their own without any complications. However, occasionally ulcers may become chronic and recur. This is probably the most common reason a patient after gastric bypass surgery may require another operation to deal with ongoing symptoms related to the ulcer.
Conclusion
If an ulcer is left untreated, it could cause serious medical problems. Besides abdominal pain, other potential complications of ulcers could be bleeding or perforation. If a perforation were to occur, typically, a patient would have severe abdominal pain that would send them to the emergency room and almost invariably require surgery. Yet, it is crucial to note that perforation occurs in ~0.85% of post-op patients.
Despite the low risk of developing an ulcer after bariatric surgery, if you experience stomach discomfort or pain post-operatively, you need to make an appointment to see your bariatric surgeon so they can properly diagnose you.
This article was originally published on the Bariatric Centers of America website.











